In Guinea, West Africa, February is the dry season; a dusty haze, stirred by the northeasterly harmattan winds, thickens the air. This year, the winds were harbingers of ill omen. That same month, Guineans began falling ill with symptoms ranging from fever, vomiting and diarrhea to muscle and joint pain and headaches. Some developed red eyes and a measles-like rash. Others bled internally, or from body openings. Death usually followed.
The ill winds continued a sweep south into Liberia and Sierra Leone, with more and more people falling sick. Within a month, international medical experts had confirmed Ebola virus disease (EVD), formerly known as Ebola haemorrhagic fever, which has a fatality rate of up to 90 percent. It was subsequently determined to be an Ebola virus of the Zaire strain, first seen in Central Africa and believed to originate in animals and likely transferred to humans via the consumption of bush meat. (Fruit bats, eaten dried or in a spicy soup, are the most likely reservoir species for the virus, reports the United Nations.) Organizations such as Médecins Sans Frontières (MSF) sent personnel like Dr. Tim Jagatic, a tropical disease specialist from Windsor, Ont. to set up field hospitals in West Africa to treat the growing number of patients.

Médecins Sans Frontières is one of several international NGOs trying to help West Africans survive the deadliest Ebola outbreak in history, which has killed more than 1,000 people. Photo credit: Sylvain Cherkaoui/ Médecins Sans Frontières
At deadline, the World Health Organization confirmed more than 1,000 deaths from EVD, which had swept into Nigeria. Physicians like Jagatic and other health practitioners have worked doggedly to try to save as many of the stricken as they could. Because EVD is highly infectious, anyone involved with the patients has to don gloves, masks and goggles and follow strict disinfection protocols to avoid contracting the virus themselves. Since there is no cure, the afflicted have been treated with antibiotics, fluids and food, giving their immune system time to rally against the virus. By deadline, however, the disease was “far from being under control,” MSF reported, and many more deaths were expected to add to an epidemic already regarded as the worst outbreak of Ebola in history.
In such cases, hope for a vaccine or a new drug to alleviate the widespread suffering becomes a topic of discussion. A key part of the conversation is biopharmaceutical company Tekmira Pharmaceuticals Corp., headquartered in a modest glass and concrete structure in a business district in Burnaby, BC. Halfway around the world from Africa, Tekmira is nonetheless inextricably linked to the region due to its revolutionary advances in antiviral therapies.
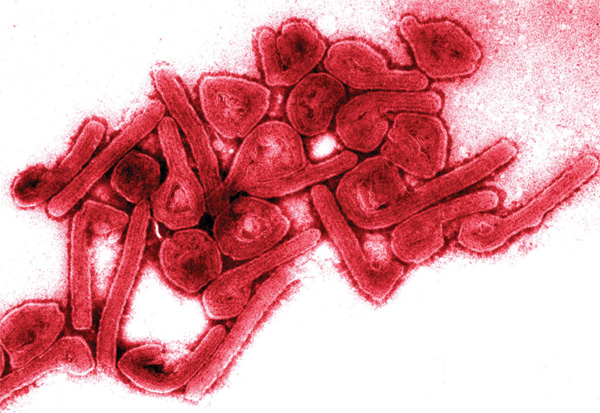
Tekmira Pharmaceuticals is also developing a therapeutic against the Marburg virus, which is similar to Ebola. Photo credit: Tom Geisbert, UTMB Health
In the past decade, Tekmira — a publicly traded company with 100 staff members and a market capitalization of about $250 million — has emerged as one of the world leaders in RNA interference (RNAi) therapeutics. This area of research is rooted in the late 20th century work of American scientists Andrew Fire and Craig Mello. (The pair won the 2006 Nobel Prize in Physiology or Medicine for their work.) In plants and animals, expressing a gene means transcribing it from double-stranded DNA into single-stranded RNA, called messenger RNA (mRNA). This molecule serves as the template to create a protein that is responsible for the biological effect of the gene. In the 1980s, scientists discovered how to manufacture their own DNA sequences that would bind to the mRNA or destroy it. The idea was to be able to silence a gene by “shooting the messenger.” Unfortunately, the technique only worked well in simple organisms. It wasn’t until the late 1990s that a series of elegant experiments conducted by Fire and Mello worked out the more complex RNA-based biochemical machinery used to silence genes in higher animals.
By 2001 it was clear that for complex organisms, the key to gene silencing was not single strands of RNA but double-stranded RNA molecules. These double-stranded sequences came to be known as small interfering RNA, or siRNA, while the overall process is RNA interference, or RNAi.
Tekmira quickly embraced the ground-breaking discovery, initiating its own RNAi research. “The lights started to go on for us and we began to imagine all possible therapeutic possibilities,” says president and CEO Mark Murray, a biochemist and molecular biologist. (Murray was a Damon Runyon-Walter Winchell Post-doctoral research fellow at the Massachusetts Institute of Technology at the same time Fire was an MIT graduate student.) “There was now an opportunity to eliminate from cells a protein or function that you believed was associated with disease,” Murray says.
Designing double-stranded siRNA sequences to interfere with a given gene is easy enough. The problem is that you can’t simply inject them into an animal and hope for the best — you need a delivery system. “In the early years of Tekmira we appreciated that to deliver a new kind of molecule — such as a nucleic acid molecule — that the rules of how to create a lipid nanoparticle had to be reinvented. So we set about doing that,” says Murray, tanned and casually dressed in jeans and a striped business shirt.
The ensuing decade saw an acceleration of Tekmira’s research into lipid nanoparticles (LNPs) for the delivery of macromolecules or nucleic acid molecules to target cells. Today, the technology allows RNAi therapies to be administered intravenously, with the siRNA molecules encapsulated in tiny particles of lipids, which travel through the bloodstream to where they need to go. LNPs are designed to accumulate at disease sites, such as cancerous tumours. Through the process of endocytosis, LNPs enter the cells and release their cargo, which destroys mRNA and silences genes.

Tekmira Pharmaceuticals’ patented lipid nanoparticle technology delivers RNA interference therapeutics into mammalian cells to combat disease. Photo credit: Tekmira Pharmaceuticals
Sound simple? It’s not. Tekmira has a dedicated team of lipid chemists and LNP formulation experts who work closely with the company’s biologists. These lipid researchers continue to develop novel lipids specifically for the purpose of RNAi delivery. Rather than using combinatorial chemistry, the lipid chemistry approach is done via what Murray calls “rational design.” siRNA sequences are large molecules and Murray says that the stability of the lipids play an important role in therapeutic delivery. These particles are designed to circulate in the bloodstream and support cellular uptake so that the RNAi trigger molecule isn’t instantly destroyed. Rather, they “fuse with the cell’s endosomal membrane and deposit the RNAi trigger molecule into the cytoplasm where the cell’s natural RNA silencing machinery, the RNA Induced Silencing Complex, or RISC, is located,” Murray says. (Tekmira is currently collaborating with Monsanto Company to apply RNAi therapeutics to plants, however, the delivery challenges are quite different, requiring more high throughput strategies, Murray adds.)
Tekmira’s RNAi innovation is possible thanks in part to the Human Genome Project, which identified and mapped human DNA. DNA contains the body’s genetic information, but relies upon messenger RNA (mRNA) to carry its protein-forming message into a cell’s cytoplasm for synthesis or processing. Diseases are often caused by either too much or an insufficient amount of a specific protein.
This cellular mechanism is harnessed by introducing into the cell an RNAi trigger, which is a molecule that allows the cell’s RNAi machinery to recognize the target mRNA. Tekmira has designed its RNAi triggers to eliminate the mRNAs encoding proteins associated with negative outcomes. This technology can also be deployed to fight viral infections. While viruses don’t make their own mRNA, they co-opt the biochemical machinery of their host cells to do so, thus RNAi “can eliminate proteins encoded by viral genes that are required for viral replication,” says Murray.

Tekmira Pharmaceuticals CEO Mark Murray. Photo credit: Tekmira Pharmaceuticals
Although Tekmira is creating RNAi products for a variety of ailments, one disease in particular locked onto its radar in the past few years — Ebola. Extremely virulent — the death rate among animals is virtually 100 percent — Tekmira saw the virus as a possible “validation for how effective our technology could be,” Murray says. Tekmira began collaborating on the development of an Ebola therapeutic with personnel from the US Army Medical Research Institute for Infectious Disease based in Fort Detrick, Md. The research was so promising, the US Department of Defense awarded Tekmira a $140 million contract to develop an Ebola therapeutic. Experimentation was carried out on rhesus macaque monkeys, used successfully in the past for the development of rabies, smallpox and polio vaccines. Ensuing tests on macaques showed Tekmira’s Ebola RNAi therapeutic, delivered via LNP, to be 100 percent effective against the Zaire strain of Ebola. “We certainly expected it was going to work but we were quite amazed we got such profound efficacy; that had never been done before,” says Murray. The results were published in a 2010 issue of The Lancet.
Tekmira currently is waiting for the green light from the US Food and Drug Administration (FDA) to continue Phase I clinical studies on humans to assess the safety of its Ebola therapeutic, called TKM-Ebola. The drug is being tested on healthy humans — not those afflicted with Ebola, says Murray. “This trial is unique. It represents the first RNAi study involving the daily treatment of healthy volunteers.” In the next portion of the study, the subjects will gradually receive increasing doses of TKM-Ebola until they receive an amount equal to what would be given to sick patients, Murray says.
The trial complements one this past May showing that small doses of TKM-Ebola were well tolerated by humans. Hence, Murray is disappointed but pragmatic about a delay this past July by the FDA to stop further testing until some drug testing protocols are refined. “It will slow the development of the drug which is unfortunate,” Murray says. Nonetheless, “the US government is very excited about it; they are quite committed.” (At deadline, due to West Africa’s dire medical emergency, the FDA partially lifted its clinical hold, allowing Tekmira’s TKM-Ebola therapy to be used on infected individuals.)
Today, Tekmira’s antiviral product line using LNP technology includes therapeutics for another highly infectious and virulent hemorrhagic fever called Marburg virus, which has affected populations in Angola, Uganda and the Democratic Republic of the Congo since the late 1990s. Tekmira reported this past April that its TKM-Marburg therapeutic prevented illness in non-human primates 72 hours after the animals were infected with the virus.
Tekmira is also utilizing LNP-delivered RNAi as a treatment for chronic Hepatitis B infection, which causes 600,000 deaths worldwide annually and is up to 100 times more infectious than HIV. As well, the company is researching development of an agent to address alcohol use disorder by turning off an enzyme in cells called aldehyde dehydrogenase 2 (ALDH2), which is involved in alcohol metabolism. Turning off the protein produces a byproduct called acetaldehyde that has numerous negative side effects and thus works as a deterrent. (The therapy has been successful in rats.)
Finally, Tekmira has developed an RNAi cancer therapeutic called TKM-PLK1. Polo-like kinase 1 (PLK1) is a natural enzyme that regulates the cell cycle but is overexpressed in tumour cells. TKM-PLK1 is being used to directly target the PLK1 in patients with advanced solid tumours.
One of the benefits of RNAi is that it doesn’t need to lock on to a target. “If you are trying to target something like the PLK1 enzyme in a tumour cell your RNAi trigger molecule is exquisitely specific for only that enzyme,” Murray says. “It’s only going to attack a cell where that enzyme is expressed.” The RNAi’s efficacy is enhanced by the footloose nature of LNP; it will go everywhere and anywhere in the body — similar to small molecule drugs — helping ensure the RNAi drug ends up where it is needed.
Tekmira is playing “a central role in bringing RNAi to reality,” Murray says. “We really enabled the field to develop by bringing the technology to convert the idea into therapeutic products. We are recognized as having made seminal contributions and that’s the thing we’re most proud of.”
And although the company’s products “are still several years away from approval and commercial success, we are well on our way,” Murray adds. It is a goal and destination that the many health practitioners and vulnerable peoples around the world are looking forward to as well.
