Infants born prematurely face a variety of challenges to their survival, starting with the simple act of breathing. It has taken medical researchers decades to understand and address a deficiency that compromises the lungs of infants, a problem that can be resolved with a product derived from the lungs of beef cattle. Now researchers at the Lawson Health Research Institute in London, ON, have helped to develop a synthetic version of this product aimed at broadening its use.
This crucial agent is a surfactant that enables our lungs to carry out their vital work as an interface between the air around us and the complex assortment of tissues that make up the bloodstream. Delicate sacs line the inner surface of these organs, which must contract and expand as the air pressure changes with each breath. By reducing the surface tension on these sacs, this lipoprotein complex facilitates their expansion and contraction, which is essential to diffusing oxygen from the atmosphere to blood in the body.
It was not until the early 20th century that scientists realized the critical role of surfactant in breathing; by the 1950s this research had revealed how its absence in neonatal infants was a leading cause of death. In the 1980s, pioneering work at Lawson by Western University investigator Fred Possmayer isolated bovine lipid extract surfactant (BLES) from cattle lungs, yielding a treatment that could be sprayed into the lungs of these newborns to save their lives.
That discovery, which was hailed by the Council of Ontario Universities as one of the top five scientific breakthroughs made in the province, became the foundation for BLES Biochemicals, a London-based firm that supplies this animal-derived surfactant to neonatal care clinics around the world.
While there have been no problems related to the production and application of BLES, teams at Lawson and Stanford University in California have been exploring the prospect of generating this surfactant synthetically. This approach would make it possible to offer it in the larger volumes that are necessary to treat breathing problems in adult patients.
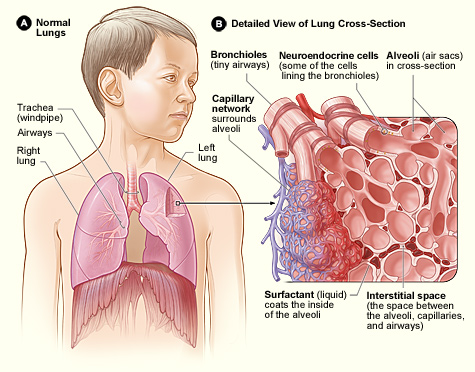
The anatomy of the alveoli, which enables gaseous oxygen to enter the bloodstream with each breath. Photo credit: National Heart Lung and Blood Institute
“We met the Stanford researchers at a conference a couple of years ago and they were interested in our lab’s capability,” says Lawson scientist Ruud Veldhuizen, referring to his facility’s long-standing expertise with laboratory rats for the study of lung surfactant.
The findings from this collaboration appeared in a recent paper for the journal Scientific Reports that details the synthetic surfactant’s use of peptoids to replace the natural polymers found in BLES.
“In these peptoids the side chains of amino acids are bound to the amine group rather than a carbon group” explains Veldhuizen. “The idea is that these protein mimics, combined with lipids, can produce a consistent synthetic surfactant”.
He adds that if the output of the synthetic version can exceed that of BLES, it could offer an improved means of treating other diseases such as pulmonary pneumonia. This bacterial infection affects the area of the lung that would be treatable with surfactant, making this material a highly efficient delivery mechanism for drugs to neutralize this threat.
“This synthetic material will make that kind of application a bit easier,” concludes Veldhuizen. “We can design its molecular structure in a way that minimizes the possibilities of interactions between a drug product and the surfactant itself.”
